Cervical headaches
(headaches referring from the neck)
I would like to share with you our view on cervical headaches (headaches referring from the neck) . The following is a summary of a discussion on the traditional understanding of migraines and tension-type headaches by Dean Watson, a leading musculoskeletal physiotherapist in treatment and research in cervical headaches.
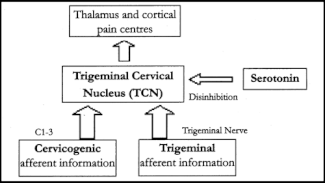
The medical model emphasizes different headaches as separate entities based on subjective features, yet there is evidence to suggest that headache is underpinned by a common mechanism, that the various types of headaches are not separate, distinct idiopathic entities. The 'continuum model' hypothesis asserts that all benign recurring headaches are driven by a similar process or common factors. Nelson (1994) has proposed this model incorporating a three-factor system (Figure on the left). At the center of this model is the Trigeminal Cervical Nucleus (TCN), its activity affected by three factors: trigeminal information, information from the cervicogenic field, and serotonin. Serotonin acts on the TCN to suppress transmission of nociceptive information. This model proposes that benign recurring headache sufferers may have varying contributions from each dimension accounting for the different presentations of headache. Cady et al (2002) have demonstrated that the similarities between migraines and tension-type headaches outweigh the differences and propose that they share a common pathophysiology. Their 'convergence theory' of primary headaches relates features of an evolving headache to current pathophysiological models. They suggest that there is a common headache process and it depends on where this escalating process is interrupted. If interrupted in the early stages, it's a tension-type headache, however, if the process continues uninterrupted, migraine results. This is similar to the continuum theory. The medical model has traditionally disparaged pathology in the cervicogenic system as having a principal role in benign recurring headaches. However, it seems logical and reasonable that chronic noxious information transmitted by cervicogenic pathways could evoke a threshold, lowering central response and therefore magnifying minor or normal events in the trigeminal field and interpreting it as noxious. In this case, cervicogenic dysfunction has the potential to be causative of a range of migraine/headache conditions. The challenge, as clinicians, is to recognize those patients in whom cervicogenic dysfunction is a key player as it cannot be done from subjective feature alone. While it is irresponsible to treat irrelevant cervicogenic dysfunction in migraine/headache conditions, it is also irresponsible (irrespective of the diagnosis) not to examine the necks of benign recurring headache sufferers in an unknown pathophysiology environment of migraine and other forms of headaches. How much longer do we accept the notion that 'whilst we do not know what causes migraine, it can't come from the neck'? The medical model of headache describes a set of symptoms which whilst may be useful for scientific researchers, provides little direction for clinicians in regard to optimal management.
Luck LI
Musculoskeletal Physiotherapist
