Crisis Plan Series
lumbar (low back) lordosis
Acute lower lumbar (low back) disc injury could be extremely painful and debilitating. The patient must clearly understand the source and cause of and therefore the severity of the condition so as to promote recovery and prevent future aggravations. Other than the required medications, the Crisis plan for such condition includes immediate relief of the spine from weight bearing, especially sitting, and positioning of the spine in its best alignment.
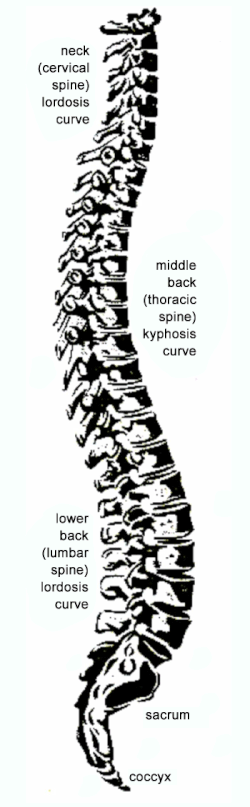
The diagram indicates the best anatomical alignment or correct posture of the whole spine. Note that the lumbar lordosis, a hollow or a S-curve in the lower back, should be maintained in all positions such as lying, sitting or standing and walking. Maintaining such lordosis will help to relief pressure in the disc, prevent further posterior (backward) disc protrusion and keeping the lumbar spine in its strongest alignment. In case of very severe and irritable condition, the amount of inflammation may make maintaining such lordosis painful. The patient may feel a lot more comfortable slouching or curling up. Although short-term relief is achieved by forward bending, it actually causes further damage and is apparent in the difficulty of straightening up from such positions and the loss of lordosis in many chronic (long-standing) low back pain patients. The patient should be advised to maintain lordosis as much as possible but just short of pain. Supine (face up) lying is best but a roll up towel under the lower back may be helpful to maintain lordosis and to give some support. Sitting should be avoided as disc pressure may increase by 50% comparing with standing and much more comparing with lying. This should be emphasized to the patient as sitting equals resting for most patients. It is also more difficult to maintain lordosis in sitting. A back brace may not be a bad idea in very painful cases, especially when time off work is not possible. Heat may help to relax muscle spasms. Specific mobility exercises could also be given in day one but only after full assessment to decide the best one/s to give as some may actually aggravate the condition. It is therefore difficult to specify these exercises here but most initial exercises may involve gentle rotation (turning) or self-traction (lengthening of the back) as far as just short of pain. The patient is also advised to get up and walk a little as much as comfortable. No matter how severe and irritable it is, there are always gentle specific hands-on mobilization techniques available to help. You may probably like to leave such hard work to the musculoskeletal physiotherapists.
The diagram indicates the best anatomical alignment or correct posture of the whole spine. Note that the lumbar lordosis, a hollow or a S-curve in the lower back, should be maintained in all positions such as lying, sitting or standing and walking. Maintaining such lordosis will help to relief pressure in the disc, prevent further posterior (backward) disc protrusion and keeping the lumbar spine in its strongest alignment. In case of very severe and irritable condition, the amount of inflammation may make maintaining such lordosis painful. The patient may feel a lot more comfortable slouching or curling up. Although short-term relief is achieved by forward bending, it actually causes further damage and is apparent in the difficulty of straightening up from such positions and the loss of lordosis in many chronic (long-standing) low back pain patients. The patient should be advised to maintain lordosis as much as possible but just short of pain. Supine (face up) lying is best but a roll up towel under the lower back may be helpful to maintain lordosis and to give some support. Sitting should be avoided as disc pressure may increase by 50% comparing with standing and much more comparing with lying. This should be emphasized to the patient as sitting equals resting for most patients. It is also more difficult to maintain lordosis in sitting. A back brace may not be a bad idea in very painful cases, especially when time off work is not possible. Heat may help to relax muscle spasms. Specific mobility exercises could also be given in day one but only after full assessment to decide the best one/s to give as some may actually aggravate the condition. It is therefore difficult to specify these exercises here but most initial exercises may involve gentle rotation (turning) or self-traction (lengthening of the back) as far as just short of pain. The patient is also advised to get up and walk a little as much as comfortable. No matter how severe and irritable it is, there are always gentle specific hands-on mobilization techniques available to help. You may probably like to leave such hard work to the musculoskeletal physiotherapists.
Luck LI
Musculoskeletal Physiotherapist
Musculoskeletal Physiotherapist
